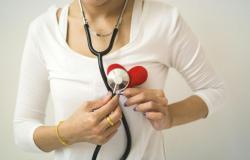
More and more is becoming known about the molecular background of pigment diseases such as vitiligo and melasma. This leads to new insights into treatment options. Dermatologist Dr. David Njoo specializes in vitiligo and melasma and talks about the developments.
Pigment disorders involve too much or too little pigment, says Njoo. “There are different clinical classifications. The most commonly used classification distinguishes between congenital and acquired pigment diseases and between local and generalized spots on the body. But within the classifications there are many hundreds of pigment disorders, also as part of another systemic disease.” Njoo has been treating patients with pigment disorders for about 2 decades. At the beginning of this century, he obtained his PhD from the University of Amsterdam on the treatment of vitiligo. He is currently a dermatologist at the Laser Clinic East Netherlands (HELON) and he has a skin and laser clinic in Amersfoort (davidnjoo.nl).
Vitiligo
The main category of conditions with too little pigment is vitiligo. This occurs in both people with light and dark skin, but it is less noticeable with light skin. The most important physical complaint is burning of the skin due to the sun because there is less pigment to block the sun’s rays. If you burn frequently, there is a risk of skin cancer, so it is important that the diagnosis is made and that patients are advised about lifestyle habits. Until the beginning of this century, vitiligo was seen as an autoimmune disease, Njoo knows. Treatment was therefore with a broadly acting immunosuppressant, locally or systemically. “But the pigment reserves in the skin eventually run out. Then the pigment will not return and treatment is no longer useful.”
When more became known about psoriasis at the beginning of this century, TNF inhibitors came onto the market to specifically block inflammatory responses. “Other inflammatory conditions benefited from this development,” says Njoo. “For example, atopic eczema and alopecia areata. And vitiligo is also now considered a chronic inflammatory condition. A lot has become known about the mechanisms behind this.”
Signaling proteins
There is not yet a biological available for vitiligo that can remove serum interleukins, as is the case with psoriasis. But there are developments in the field of so-called intracellular ‘small molecules’. Njoo explains: “These are small protein molecules that transmit signals in the cell and thus activate the cell. Many signaling proteins have been identified for inflammatory skin conditions, including vitiligo. Interferon-γ in particular appears to play a role, as part of the JAK signaling pathway with Janus kinase enzymes involved in inflammation and defense. Inhibiting the JAK signaling pathway is now receiving a lot of attention in vitiligo.” Several JAK enzymes are now known. “It is now possible to locally slow down this with a skin cream,” says Njoo. “We are currently in the process of registering ruxolitinib for the treatment of vitiligo. It is already on the market in the US, but we cannot yet officially prescribe it here. It is an expensive drug: approximately 1,000 euros for a 50 gram tube. That price still needs to be lowered. The drug would be a breakthrough, because with this cream we may be able to stop the disease process. There are side effects, because the JAK signaling pathway is necessary for protection against, for example, respiratory infections. Typical side effects of JAK inhibitors are headaches, runny nose and herpes infections.”
In the US, the effects of ruxolitinib are favorable, but patients must take the drug for at least six months. “So we have to encourage them to persevere,” says Njoo. “Studies in Amsterdam with this product show that the effect does not decrease after 1 year of application. Perhaps it is a lifelong treatment. There are also oral JAK inhibitors being researched, which often have fewer side effects. Some of these are already available for the treatment of atopic eczema.”
Melasma
An example of a disorder with too much pigment is melasma. This does not immediately cause physical complaints, but can be cosmetically drastic. Njoo sees melasma increasing, especially in people with colored skin. Various enzyme inhibitors are available to slow down the production of pigment, but slowing down is not sufficient. There are also bleaching creams to treat melasma, but it comes back after stopping them. Njoo: “We need to do much more when treating melasma. But the available treatments are not reimbursed and are therefore difficult to access for patients. Treatments are only given outside the hospital.” Until about 10 years ago, melasma was seen as a disease of the pigment. But it is probably a skin problem due to sun damage. “We see all kinds of effects in the dermis. When treating melasma, the practitioner must therefore also repair the dermis. In addition to pigment cells, other cells are also involved, such as blood vessel endothelial cells, fibroblasts and keratinocytes.”
Combination therapy
In melasma, the basement membrane is severely damaged, Njoo knows. As a result, the pigment produced does not remain in the epidermis, but goes directly to the layers below. “It is difficult for local resources to achieve this. That is why we have to rely on so-called ‘energy-based devices’, or EBDs. There are many developments in this regard. Treatment is done with, for example, light pulses, laser or ultrasound and aims to rejuvenate the skin. That’s what we want with melasma. With EBDs you can, among other things, tackle sun damage, make the skin supple again and reduce excess blood vessels.” According to Njoo, treating melasma with a bleaching cream alone is too limited. “At least 1 bleach and at least 1 EBD are needed. So not monotherapy, but a combination.”
There are plenty of developments in the treatment of pigment disorders. Njoo expects a new drug against vitiligo in a few months. With regard to melasma, the development of safe EBDs and bleaching creams and targeted sunscreens continues. “And there may also be JAK inhibitors against melasma. We know better and better which key proteins play a role.”
Mast cells
Research has made it clear that mast cells also play a role in melasma. These are found in abundance in affected areas and the question is what they are doing there. “At the moment it is only clear that they are released locally in the skin during sun damage,” says Njoo. “But how do you tackle this in a targeted manner with melasma? We do not know yet. Oral antihistamines have no effect. Studies are now being done with topical antihistamines. This may offer opportunities to reduce the number of mast cells. Because melasma is now seen as a sun damage problem, patients are advised to avoid the sun and use sunscreen, especially against UV-A.”